Invoicing for Benefits and Medical TPAs
TPA Stream helps Benefits and Medical TPAs turn scattered billing and admin data into clean, accurate employer invoices, using the systems your operations team already relies on.
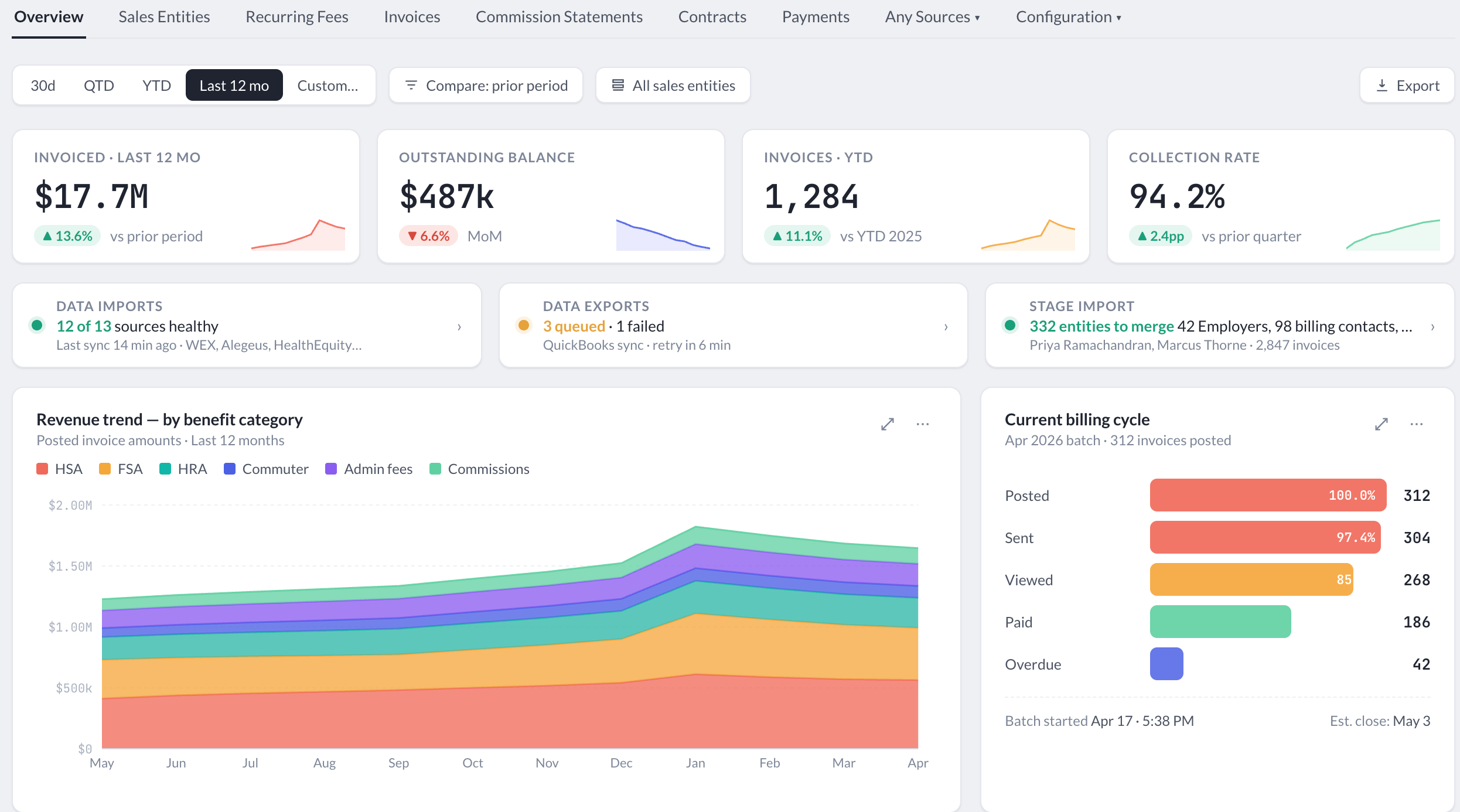
Why invoicing is harder than it should be
Most TPAs are pulling billing data, eligibility records, and contribution information from multiple systems — then reconciling it by hand before an invoice can go out, and then manually entering the results into their accounting platform. The result is slow cycles, avoidable errors, and operations teams spending too much time on work that should be automated.
For Benefits TPAs, this is compounded by the fact that CDH and COBRA administration often run on separate platforms — and enrollment data frequently originates in a system like Employee Navigator before it ever reaches those platforms. TPA Stream works across all combinations, so your invoicing workflow doesn't have to treat them as separate problems.
Billing and admin data spread across multiple platforms — including separate CDH and COBRA systems — with no single source of truth.
Slow invoice cycles and avoidable errors caused by hand-matching data across systems.
No way to bring it all together without building something yourself or relying on workarounds.
How TPA Stream helps
TPA Stream connects to the platforms your team already uses and pulls the data needed to build accurate employer invoices — without replacing your existing systems or adding a heavy implementation.
Operations teams get cleaner output with less manual work. Employers get invoices that are easier to reconcile. And your team spends less time chasing down data before billing runs.
Pull billing and admin data from multiple sources into a single, unified invoicing workflow.
Cut down the reconciliation work that slows operations teams and introduces invoice errors.
Accurate employer invoices on a consistent cycle, without the manual scramble.
Built for how TPAs actually work
TPA Stream supports both Benefits and Medical TPA invoicing workflows, with integrations for the platforms each side of the market relies on.
Benefits TPAs
TPA Stream integrates with the systems Benefits TPAs use to manage CDH and COBRA — pulling the data needed to generate cleaner employer invoices without manual consolidation, regardless of which combination of platforms you run.
Enrollment: Employee Navigator
CDH: Alegeus WCA · WEX · Elevate
COBRA: Alegeus WCC · WEX COBRA
Explore Benefits TPA SolutionsMedical TPAs
TPA Stream supports Medical TPA invoicing workflows by connecting to the platforms operations teams already work in, helping them produce employer invoices with less manual effort.
Works with: QicLink · VBA · Healthpac · Javelina
Explore Medical TPA SolutionsWhat customers say
"Very happy with how TPA Stream integrates our multiple databases into a single monthly invoice. TPA Stream offered very detailed training and continues to provide great support as needed."
— TPA Stream customer
Works with your existing systems
TPA Stream is designed to work alongside the platforms your team already depends on — not replace them. Integration is a core part of how the product works, not an afterthought.
Benefits TPA platforms
Enrollment
Employee Navigator
CDH
Alegeus WCA · WEX · Elevate
COBRA
Alegeus WCC · WEX COBRA
Medical TPA platforms
QicLink · VBA · Healthpac · Javelina
Accounting platforms
QuickBooks Online · QuickBooks Enterprise · Microsoft Dynamics GP · Sage Intacct · Oracle NetSuite · homegrown and custom systems
See TPA Stream in action
Book time with our team to see how TPA Stream can help your operations team get accurate employer invoices out the door faster.