A detailed look at a detailed invoice
Why are detailed invoices so important for Third Party Administrators to provide to their Employers
As an expert benefits administrator for COBRA and consumer-directed healthcare accounts, it is important to provide clear and detailed invoices to your employer clients. Invoices should include information about the various fees associated with each type of account, as well as instructions for payment options.
But, third party administrators often struggle to put together a detailed invoice for their employers because it’s difficult to map the participant details to the fee schedule and manage complex recurring fees. This leads to confusion for the employer and lots of back and forth between the TPA and the employer when fees are incorrect or need to be adjusted.
If you’re curious about what a detailed invoice from TPA Stream would look like, read on as we break down the key features of a detailed invoice, and how you might configure an invoice for your clients. Keep in mind, this invoice was generated in just three clicks.

The sections of a detailed invoice
This sample detailed invoice is meant to show you the level of flexibility you can achieve with an invoice. When you’re configuring your recurring fees, you have a ton of flexibility in terms of how these fees are assessed and applied, like based on the total insured employee count, based on total members in that service, bundled pricing, minimums, and more. These are just common fees that our customers use. Each fee can be configured to meet your specific needs.
The Third Party Administrator’s Logo
When you generate an invoice using Employer Invoicing, your logo is automatically included on all your invoices sent. This helps to ensure that the invoice is coming from a trusted source and helps to establish brand recognition for your company.
Total Summary Section
This section outlines all the fees assessed for that period in one easy-to-read table before getting into the detailed breakdown by fee.
Annual Renewal Fee
This is a recurring fee that is charged annually to the employer for administering the COBRA and consumer-directed healthcare accounts. The annual renewal fee covers the cost of account maintenance, compliance with federal regulations, and other administrative expenses.
One consolidated invoice includes COBRA Fees
COBRA Monthly Fee
This is a recurring fee that is charged monthly to the employer for administering the COBRA accounts. The COBRA monthly fee covers the cost of managing the COBRA accounts and ensuring compliance with federal regulations. It provides employers with the peace of mind that their COBRA accounts are being managed by a trusted administrator.
COBRA Participant Fee
This fee is billed per member based on the total number of insured employees. It covers the cost of managing consumer-directed healthcare accounts, including enrollment, claims processing, and other administrative expenses.
We’ve also seen fees configured per letter, which is an option, too.
One consolidated invoice includes CDH services
Send one invoice for all the services you provide, including COBRA and CDH.
FSA Admin Fee
This fee is charged based on the number of members who are enrolled in an FSA. It covers the cost of managing the FSA accounts, including enrollment, claims processing, and other administrative expenses. Here, you can see that with Employer Invoicing, you’re able to send your employer just one invoice for both CDH and COBRA, even if you use two systems to manage the administration like Weath care COBRA or Wealth Care Admin.
Bundled Fees
In this example, there is a bundled fee for FSA and HRA administration. This fee is charged per unit for everyone who has both an FSA and an HRA. It covers the cost of managing both the FSA and HRA accounts, including enrollment, claims processing, and other administrative expenses. Employer Invoicing supports bundled rates.
HRA Admin Fee
This fee is billed per member for managing the HRA accounts. It covers the cost of managing the HRA accounts, including enrollment, claims processing, and other administrative expenses. It also includes a monthly minimum fee, which is configurable when you add in recurring fees.
Divisional Billing
In this example, you can see the fee for HSA Administration is split between East and West divisions. The Employer Invoicing solutions supports divisional billing, too.
Based on how you bill your employers, Employer Invoicing offers a ton of flexibility for how you assess fees. Additionally, there is no other system that streamlines and consolidates billing records from multiple sources like COBRA systems and CDH administration systems offered by WEX Health and Alegeus.
Getting paid
Finally, in this invoicing sample, it says “funds will be pulled on the 15th.” We support multiple payment methods including Credit Card (would include a link to pay the invoice directly via Quickbooks) or ACH through a NACHA file. This enables our customers to get paid faster and more accurately.
Configuring the fees
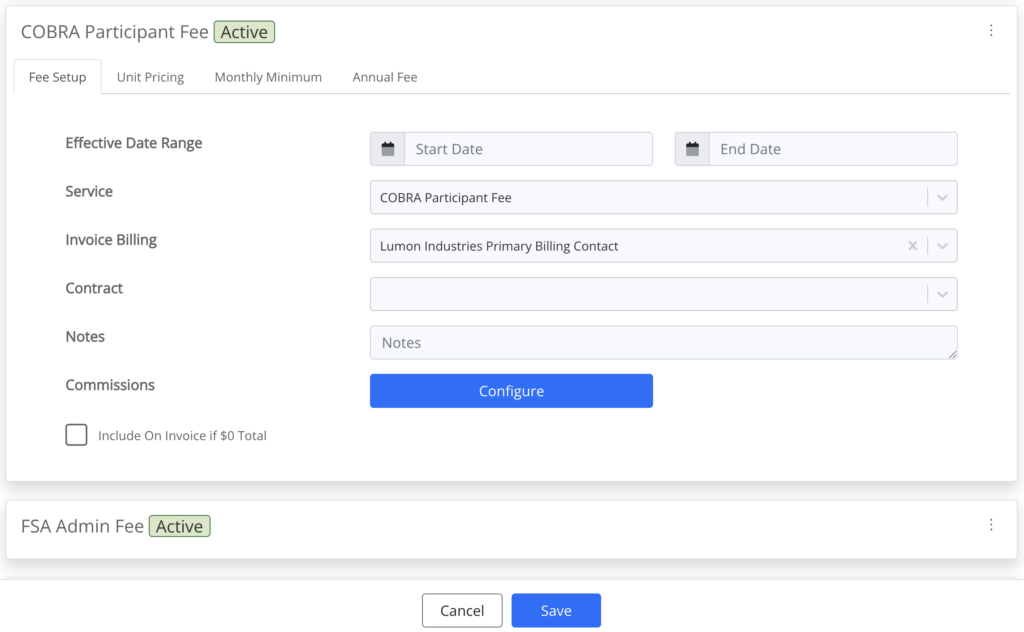
The power of Employer Invoicing lies in the Recurring Fees configuration. Each fee that you add has almost limitless options including:
- Unit pricing
- Bundle pricing
- Monthly minimums
- Annual fees
- Commissions associated with the fee
Once configured, these recurring fees just run, with very little involvement from you. We’ll help you configure these during your onboarding process.
Conclusion
To sum up, manually managing COBRA and consumer directed healthcare accounts is complex and time-consuming, and can lead to costly mistakes and a loss of trust between administrators and employers. However, TPA Stream’s Employer Invoicing automates the invoicing process, saving time and reducing errors. By using this solution, administrators can provide accurate and detailed invoices, while focusing on delivering high-quality healthcare benefits to their clients. The Employer Invoicing feature from TPA Stream is the perfect solution for administrators who want to streamline their invoicing process and ensure the best possible outcomes for their clients.


